By David P. Brungo, PT, Expert Contributor, Summerville PT & Balance Rehab for Adults
I’ve been a PT for nearly 30 years and one of the most common conditions I’ve seen is wear and tear arthritic knee pain (aka, osteoarthritis), and for good reason. Our knees take a beating over the course of our lives and we all are different with respect to how our knees hold up over time. We’re genetically predisposed to some things that work against us, such as our bone density and joint anatomy or propensity toward disease processes like obesity, kidney disease, high blood pressure or hormonal imbalances that we inherit, others are activity related, such as trauma from injuries or repetitive stress (e.g., an automobile collision, a football or cheerleading injury, a fall from a ladder, etc.), and of course some are lifestyle related, such as the destructive effects from long term smoking or alcohol, an unhealthy diet or inadequate level of exercise.
We’re all different with respect to the portfolio of variables we each have that contribute to our knee arthritis and, likewise, we each perceive and experience things differently as well as respond uniquely to the various ways for us to manage or treat the problem. We’re all different – managing knee arthritis is not a cookie cutter activity and there is no valid “apples to apples” comparison that we can use to gauge how we will experience, for example, a total knee joint replacement surgery compared to others who have had the same procedure. Yet, we do this all the time and it can really impact our decision to seek the most effective care in a timely manner.
There have been a lot of great advances in how knee arthritis can be managed. Newer medicines and improved surgical procedures and materials have developed with some really promising emerging interventions getting a lot of attention, too. And we’re learning more and more about how our lifestyle choices contribute to the big picture.
I believe the best patient outcomes are typically associated with patients who are best informed about their options when it comes time to do something about their knee arthritis. Thus, it’s imperative to do your homework. I’ll try to make that a little easier here.
Let me start by saying this: There is no magic pill – at least not yet! You will have to work toward a successful outcome and yes, pain is part of the equation but you should never be asked or expected to work beyond your tolerance.

Fortunately, there is no shortage of information available to us when we’re ready to do some homework so look for a credible resource that does a really nice job explaining the nitty gritty and summarizing your options. For example, according to WebMD, the primary goals of treating osteoarthritis of the knee are to (1) relieve the pain and (2) maximize normal and healthy mobility. Successful outcomes will typically include a combination of the following:
Weight loss: Losing even a small amount of weight, if needed, can significantly decrease knee pain from osteoarthritis.
Using assistive devices or braces: Using a cane or a walker may be necessary to provide more body support while standing or walking. There are generally two types of braces: “off loader” braces, which take the weight away from the side of the painful knee; and “support” braces, which provide external support around the entire knee.
Exercise: Strengthening the muscles around the knee makes the joint more stable and decreases pain. Stretching exercises are important to ensure that muscles are working at their optimal lengths, which helps keep the knee joint mobile and flexible with the least amount of inflammation from muscular imbalances.
Pain relievers and anti-inflammatory drugs: This includes temporary use of over-the-counter (OTC) medications such as acetaminophen, ibuprofen, or naproxen. If OTC meds don’t provide enough lasting relief, your doctor may give you a prescription for an anti-inflammatory drug or other medication to help ease the pain. Examples of these include opioid meds (oxycodone, hydrocodone, codeine, morphine) and non-opioid meds (naproxen, topical lidocaine, meloxicam, celecoxib).
Injections of corticosteroids or hyaluronic acid (HA) into the knee: Steroids are powerful anti-inflammatory drugs. Hyaluronic acid is normally present in our joints as a type of lubricating fluid. Stem cell therapy is an emerging medical intervention that’s getting a lot of attention but may not have the robust, long-term analysis on its effectiveness on all the things we’d like it to fix, such as the entire joint surface with new and healthy bone covered in a beautifully thick layer of bone-protecting cartilage!!! Sorry — we’re not quite THERE yet!!!
Alternative therapies: Some alternative therapies that may be effective include topical creams with capsaicin, acupuncture or supplements, including glucosamine and chondroitin or S-Adenosyl methionine (SAM-e).
Physical and occupational therapies: If you are having trouble with daily activities, physical or occupational therapy can help. Physical therapists can help with keeping pain and swelling under control while teaching you ways to strengthen muscles, increase flexibility around your knee and work toward restoring lost mobility. Occupational therapists teach you ways to perform regular, daily activities, such as self-care and housework, with less pain and sometimes incorporates use of assistive devices such as reachers or sock-donners.
Surgery: When other treatments don’t work, surgery is usually your next option to consider. If your doctor wants to treat the osteoarthritis in the knee with surgery, the options are arthroscopy, osteotomy, and joint replacement (arthroplasty).
Arthroscopy uses a small telescope (arthroscope) and other small instruments. The surgery is performed through small incisions. The surgeon uses the arthroscope to see into the joint space. The surgeon can remove damaged cartilage or loose particles, clean the bone surface and repair other types of tissue if those damages are discovered. The procedure is often used on younger patients (55 and younger) in order to delay more serious surgery.
An osteotomy is a procedure that aims to make the knee alignment better by changing the shape of the bones. This type of surgery may be recommended if you have damage primarily in one area of the knee. It might also be recommended if you have broken your knee and it has not healed well. An osteotomy is not permanent, and further surgery may be necessary later on.
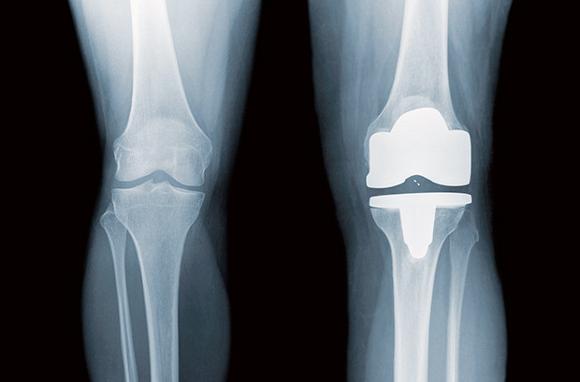
Joint replacement surgery, or arthroplasty, is a surgical procedure in which joints are replaced with artificial parts made from metals or plastic. The replacement could involve one side of the knee or the entire knee. Joint replacement surgery is usually reserved for people over age 50 with severe osteoarthritis. The surgery may need to be repeated later if the joint wears out again after several years, but with today’s modern advancements most new joints will last over 20 years. Any surgery has risks, but the results are generally very good. NOTE: Rehab following a knee joint replacement is hard work and an extended process that could take 3 – 12 months. You’ll need to be prepared mentally for the process, which can be a bit of a grind but you will be glad you kept forging on with your head down while doing whatever you need to do to keep on taking steps toward the destination — a markedly improved Quality of Life with no more knee pain! It does not have to be misery!

Stay in the Game by committing to regular exercise and do your best to maintain a healthy lifestyle.
If you’re suffering with arthritic knee pain you should talk to your doctor about your options. Your options should always be considered from a “big picture” perspective and typically will require diagnostic studies such as blood work, xrays and of course a thorough medical and physical examination that considers, among other things, your medication history, diet and lifestyle. Once you and your doctor decide which path you will take, it’s likely that you’d benefit from physical therapy whether your plan involves surgery or not. Exercise is critical and working with a physical therapist has been shown to be highly effective in managing knee arthritis before and after surgery and will help you achieve optimal functional results and maximum Quality of Life!
For more information, see: Osteoarthritis of the Knee (Degenerative Arthritis of the Knee) (found online at https://www.webmd.com/osteoarthritis/ostearthritis-of-the-knee-degenerative-arthritis-of-the-knee#1; May 19th, 2018).